When Your Child Has Coarctation of the Aorta (COA)
Your child has been diagnosed with coarctation of the aorta (COA). COA is a narrowing in the aorta. The aorta is the main blood vessel that carries blood from the heart to the rest of the body. COA can lead to worsening heart function over time and elevated blood pressure. Current treatments are quite effective for this condition.
The normal heart
The heart is divided into 4 chambers. The 2 upper chambers are called atria. The 2 lower chambers are called ventricles.
In a normal heart, oxygen-poor blood returning from the body fills the right atrium. This blood flows through the tricuspid valve into the right ventricle. The right ventricle pumps this blood through the pulmonary valve. It goes into the pulmonary artery and then to the lungs to pick up oxygen. Oxygen-rich blood from the lungs fills the left atrium. This blood flows through the mitral valve into the left ventricle. The left ventricle pumps this blood through the aortic valve to the aorta to send oxygen to the body.
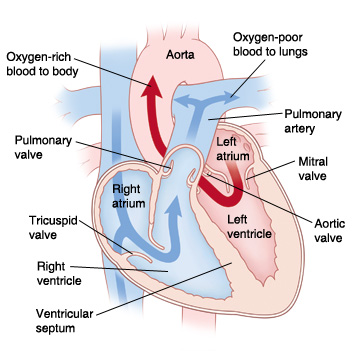 |
| In a normal heart, blood flows from the heart to the body through the aorta. |
Why is coarctation of the aorta a problem?
With COA, the left ventricle has to work harder than usual to pump blood to the body. This is because there’s reduced blood flow due to the narrowed area in the aorta. Over time, the extra work tires the left ventricle. This causes the heart muscle to weaken. It can also cause the muscle to thicken (hypertrophy). In severe cases, a child can develop congestive heart failure (CHF). This is a condition in which the heart can no longer pump blood well and meet the demand of the tissues and organs.
Blood pressure is the amount of force of blood pushing against blood vessel walls as it pumps through the body. High blood pressure (hypertension) is when blood pushes with more force than normal. Low blood pressure (hypotension) is when blood pushes with less force than normal. With COA, blood pressure is high in the upper body and less in the lower body. This is because the pressure is higher in the arteries in the area before the narrowing. These arteries send blood to the head and arms. The pressure is lower in the arteries in the area after the narrowing. These arteries send blood to the abdomen and legs. Problems with blood pressure can lead to other health problems. These include stroke, kidney failure, and intestinal damage.
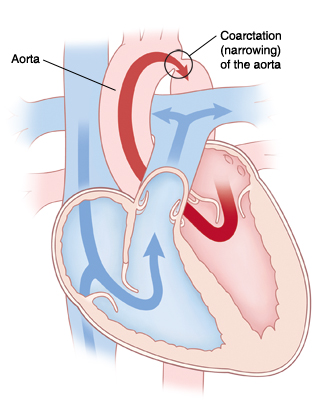 |
| With COA, blood flow to the body is reduced because of narrowing in the aorta. |
What causes coarctation of the aorta?
COA is a congenital heart defect. This means it’s a problem with the heart’s structure that your child was born with. COA occurs more often in families with a history of left-sided heart problems. It also occurs more often in children with certain genetic problems.
What are the symptoms of coarctation of the aorta?
Children with mild to moderate COA may have no symptoms at first. Babies with critical COA often have severe symptoms. Symptoms can include:
-
Heavy or fast breathing
-
Irritability
-
Infection of the intestines
-
Poor growth
-
Tiredness with exercise (in older children)
-
Cold extremities (in older children)
-
Pain in the lower part of the leg while walking (in older children)
-
Circulatory collapse (child becomes gray, cold, and the heart may stop beating)
-
Trouble feeding (in babies)
How is coarctation of the aorta diagnosed?
Sometimes, COA can be found with fetal echocardiography (fetal ultrasound) before a child is born. This is a test that uses sound waves to form a picture of the baby’s heart. This test can be done beginning at 12 weeks of pregnancy.
Often, COA isn’t found before birth. In this case, signs of a heart problem may be found during a physical exam after birth. Possible signs include high blood pressure in the arms or poor pulses in the legs.
If a heart problem is suspected, your child will be referred to a pediatric cardiologist. This is a doctor who diagnoses and treats heart problems in children. Your child may have tests such as:
-
Chest X-ray. X-rays are used to take a picture of the heart and lungs.
-
Electrocardiogram (ECG). This test records the electrical activity of the heart.
-
Echocardiogram (echo). Sound waves are used to create a picture of the heart and look for structural defects and other problems.
-
Cardiac catheterization. A thin, lighted tube is inserted into a vein and guided to the heart to view the heart's structures.
-
Cardiac MRI or CT scan. Magnetic waves or X-rays are processed by a computer to make pictures of the inside of your child’s heart.
How is coarctation of the aorta treated?
COA is treated with open heart surgery or cardiac catheterization. Surgery may be done using a number of methods. The exact method will depend on the extent of narrowing and where it is in the aorta. Cardiac catheterization is most often done on older children. Your child’s cardiologist will assess your child’s heart and talk with you about the best treatment options.
What are the long-term concerns?
-
After repair of COA, most children can be active and join in sports and physical activities.
-
Regular follow-up visits with the cardiologist are needed. The frequency of these visits may decrease as your child grows older. COA may recur in the long-term. Aortic aneurysm or widening of the blood vessel may occur in the area that was treated. More treatment may be needed when your child is older.
-
Your child may need to take medicine to treat problems such as high blood pressure. This is common in older children even after repair of COA.
-
Your child may need to take antibiotics before having any surgery or dental work for 6 months after COA repair. This is to prevent infection of the inside lining of the heart or valves. This is called infective endocarditis. Antibiotics should be taken as directed by the cardiologist.